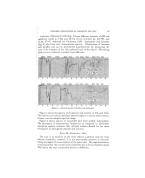
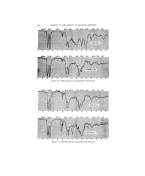
i: HYPO- AND HYPERPIGMENTATION OF SKIN 249 ?'?:: . In 1950, Grupper used H-365, p-hydroxypropiophenone, in dosage of i•:71-2 gin. daily for the treatment of Riehl's Melanosis, a condition which he ?!•:?2'::believed due to pituitary gland dysfunction (14). He claimed successful i!!771•177 results in this condition and other cases of hyperpigmentation. !:i}i} .. Following this discovery of the inhibitory effect on melanin production ?i. by the p-hydroxyphenyl derivatives, studies to determine their mode of action and therapeutic value have been attempted (Fig. 1). :? .'-, Denton, Lerner, and Fitzpatric (15) have shown by in vitro studies that ii,!.'j.'.hydroquinone and p-hydroxypropiophenone effectively inhibit the enzy- i?matic oxidation of tyrosine to dopa (the first phase of melanogenesis) by 't::•:t':measurements of oxygen uptake and quantitative analysis of unreacted tyrosine at the end of the reaction. No inhibition occurred when dopa ?•::::was used as a substrate. The monobenzyl ether did not do the same its '•:.•':• mechanism of melanin inhibition is not known unless perhaps it is con- 't• /'Vetted to hydroquinone in the skin and acts as such. Animal tests were perGrmed in which hydroquinone, monobenzylether ? •'/0f hydroquinone and p-hydroxypropiophenone were fed to guinea pigs. Depigmentation was produced. The injection of hydroquinone produced depigmentation at the site of injection after 4 weeks p-hydroxypropio- •i.::phenone showed a diffuse increase in the number of gray hairs mono- .:'-:2•: benzyl ether of hydroquinone showed no depigmentation. Clinical trials of 10-33% of monobenzyl ether of hydroquinone proved to be an effective agent in the treatment of melanin hyperpigmentation. ß }•:• Hydroquinone cannot be used locally due to its instability. p-Hydroxy- 'propiophenone has little local action. For the treatment of his cases Den- ton used a 20-30% concentration in a vanishing cream or a 20% lotion in 10 parts of alcohol and 7 parts of acetone. He claimed a low incidence of sensitivity by patch testing (15). HYPOPIGMENTATION Leukoderma, absence o{ melanin pigmentation, is a result oF incomplete melanization. Sections of skin from leukoderm•c areas do not give a posi- tive dopa reaction indicating that there may be an absence of melanocytes or that there is a faulty enzyme system. Healing inflammatory les•ons o[ the skin may result in lack ofpigment this is usually a reversible process. Congenital generalized absence of pigment is known as albinism. Idio- pathic leukoderma, vit{ligo, is the most common type seeking therapy. Until recently treatment was very ine•ective. Activation o• pigmentation is attempted with ultra-violet light which oxidizes the sulfhydryl content of the skin and helps to convert reduced melanin to its darker stage. Applica- tions o{ oil o• bergamot followed By ultraviolet lamp light is not too e•ec- tire. Spencer's technique of phenol applications is a prolonged course of therapy with variable results.
250 JOURNAL OF THE SOCIETY OF COSMETIC CHEMISTS OCH3 8-Methoxypsoralen Ammoidin Xanthotoxin o//XO, x'•/-- I /CH3 OCH2CH•---C•,cH • 8-Isoamyleneoxypsoralen Ammidin Figure 2 Since the 13th century, the Egyptians have used a powder from a plant called Ammi Majus Linn for the treatment of leukodermas. In 1947 the two active ingredients of this plant were extracted and are known as Am- moidin and Ammidin (Fig. 2). Chemically they are related to the furo- coumarins (16). The use of these drugs by Egyptian, French, and Ameri- can workers has shown that they have a specific action on vitiligo (17, 18, 20). These therapeutic agents are used orally or locally or in combination in conjunction with ultraviolet or sunlight. The local treatment consists of light application on the leukodermic areas with an alcoholic solution containing Ammoidin and Ammidin two to three times per week followed by suberythema doses of ultraviolet light. Bullous reactions may occur after the first applications but are not necessary for good results. Pigment appears as small macules with hair follicles in the center. These increase in size, joining and forming larger islands of pigmentation. It takes ap- proximately one month for the appearance of pigmentation. Internal treatment consists of oral ingestion of tablets containing Am- moidin and Ammidin. Nervousness, insomnia, and gastric complaints may accompany the oral method of therapy. EI Mofty observed good re- sults with the intradermal injection of these extracts (19). To date actual definitive therapy to reactivate melanin formation is still an experimental study. While the Ammoidin-Ammidin regime appears to be the most effective so far, it is too early to predicate over-all medical ac- ceptance until more detailed study as to side effects is observed. REFERENCES (1) Lever, W. F., "Histopathology of the Skin," Philadelphia, Lippincott (1949), pp. 6-21. (2) Ormsby, O. S., and Montgomery, H., "Diseases of the Skin," 7th ed., Philadelphia, Lea and Febiger (1948), pp. 15-72. (3) Lerner, A. B., and Fitzpatrick, T. B., "Biochemistry of Melanin Formation," Physiolog. Reviews, 30, 91-126 (1950). (4) Bloch, B., Das Pigment, in Jadassohn, J., "Handbuch der Haut und geschlechts- krankheiten," Vol. 1, Berlin, Julius Springer (1927), pp. 434-541. (5) Masson, P., "Pigment Cells in Man in Biology of Melanomas," Special Publica- tions, Vol. 4, New York Academy of Sciences (1948), pp. 15-51. (6) Fitzpatrick, T. B., Lerner, A. B., Calkins, E., and Summerson, W. H., "The Occurrence ooe Tyrosinase in Horse and Fish Melanomas," ,Proc. $oc. Exptl. Bid. and Med., 75, 395-398 (1950).
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)