102 JOURNAL OF THE SOCIETY OF COSMETIC CHEMISTS The current study was designed to examine, using more precise methodology (flow cytometry), the density of the Class II major histocompatability (MHC) Ia antigen on epidermal immune cells that had been previously treated in intact epidermis with various antioxidants or a biologically relevant molecule, arachidonic acid. It has been previously documented that the density of the Ia antigen membrane marker correlates with the intensity of epidermal immune reactivity (e.g., allergic contact dermatitis (1,3,5). We suggest that the described methodology may be useful as a sensitive screening technique for ascertaining whether common and/or new antioxidants used in medications and/or cosmetics may exacerbate common immune-mediated dermatoses such as allergic contact dermatitis. MATERIALS AND METHODS Four-to-six-week-old male DBA/2 d and C57BL/6 b mice were obtained from Jackson Laboratories (Bar Harbor, Maine) and were housed in University facilities, four to six per cage with free access to water and Purina Mouse Chow © . The animals were exposed to an ambient 12-hour light:dark photoperiod. The experiments were performed at least twice and produced similar results. IN VIVO EXPOSURE TO MBEH AND AA DBA/2 mice were treated topically with either 50 }zl of 20% MBEH in 95% ETOH or 0.05% and 1.0% AA in DMSO:H20 (1:1) applied to the dorsal pinnal epidermis daily for five days. Control animals were topically treated with 95% ETOH diluent or the DMSO:H20 (1:1) diluent. On day 6, treated and diluent control ears were surgically excised and epidermal suspensions were prepared and subjected to fluorescent-activated cell sorting analysis as described by others (6,8,9) with modifications. IN VITRO EXPOSURE TO AA, BHT, BHA 4 x 105 viable unenriched epidermal cell suspensions were prepared and plated in 24-well Linbro polystyrene tissue culture plates. To the unenriched epidermal cells, various concentrations of AA, BHT, and BHA were added in complete RPMI 1640 cell culture media supplemented with 1.5 }zg/ml of indomethacin. A series of pilot experi- ments was performed at various concentrations to determine the in vitro effects of the specific phenols BHT, BHA, and AA. The maximum biological effects were produced by the following solutions: BHT, 2.5 !zg/ml BHA, 5 !zg/ml and AA, 66 ng/ml and 666 ng/ml therefore, these concentrations were used throughout the studies. Following 48 hours of incubation at 37øC in 5% CO2, the cells were harvested, washed in com- plete 1640 RPMI medium, and incubated with appropriate primary and secondary fluorochrome-conjugated antibodies at 4øC (8,9). Treated and control epidermal cell preparations were then subjected to FACS analysis and the density of Ia expression quantified. To ensure that the cells were Langerhans cells and not keratinocytes which can also express the Ia membrane antigen in allergic contact dermatitis, unenriched epidermal cell suspensions were double stained with the Ia and Fc receptor antigens. The antigens were then conjugated with appropriate secondary antibodies, specifically fluorescein isothiocyanate and streptavidin phycoerythrin red.
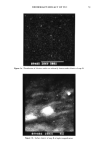
ANTIOXIDANTS IN IMMUNITY 103 RESULTS TOPICAL ADMINISTRATION OF MBEH: IN VIVO ANALYSIS Figures la and lb depict the results of experiments in which mice were treated for five days with 20% MBEH or 95% ethanol (diluent) to dorsal pinnal epidermal surfaces. On day 6, the ears were surgically excised and the cells were subjected to fluorescent-acti- vated cell sorting using a FACS 440 (Becton Dickinson, Mountain View, CA). 30,000 events (e.g., cell parameters, of fluorescein intensity and size) were examined. 1.4% of the cells proved to be Ia + Langerhans cells in the control (diluent) versus 3.3% in the MBEH treatment group (see Figures la and lb). Normal Langerhans cell density, cells/ mm 2, makes up approximately 2% of the total epidermal cell density in this particular strain of mice. In addition, the mean fluorescence intensity increased from 69.51% (control) to 72.99% (treatment) (Figures la, lb). These results corroborate our earlier in vivo light microscopy experiments in that the numbers of Langerhans cells, i.e., density of cells/mm 2 (1), and the expression of the Ia antigen marker are increased following topical treatment with the common antioxidant MBEH. IN VITRO FACS ANALYSIS OF BHT, BHA AND AA Table I shows the results of experiments in which unenriched epidermal cell suspensions were exposed to various concentrations of arachidonic acid alone or with BHA, BHT, and the control diluents. Following 48 hours of incubation, the cell preparations were harvested and subjected to FACS analysis to quantify changes in Ia+ antigenic cell membrane expression. The results demonstrate that there is an apparent biphasic effect following exposure to low or high doses of AA, with or without the antioxidants BHA and BHT. There was a significant decrease (p • 0.05) (Student t-test) in the quantity of Ia + expression from unenriched epidermal cell suspensions following exposure to a large dose of arachidonic acid. Further, the addition of indomethacin (IND) to the cell culture wells containing high doses of AA could restore Ia antigenic expression to con- trol values (data not shown). These data corroborate our earlier in vivo studies in which a large 1% AA concentration decreased the number of Ia + Langerhans cells as well as CHS responsiveness, while a more dilute concentration of 0.05% AA could increase both LC density (cells/mm 2) and enhance the CHS or allergic contact dermatitis re- sponse in several mice strains (1). DISCUSSION It has been reported earlier that the mechanism by which MBEH, BHT, and BHA may alter the Ia antigenic marker expression in epidermal cells is via the arachidonic acid/ prostaglandin biochemical pathway (1,10). The quenching of the radical oxygen mole- cule in this pathway by these common antioxidants irreversibly inhibits the cyclooxy- genase enzyme, thereby affecting arachidonic acid metabolism directly and/or indirectly via the oxidation of AA into its products, namely the prostaglandins and leukotrienes. Other investigators have documented that common antioxidants can affect systemic immune reactivity (11, 14). However, there has been a paucity of studies regarding the role of topically applied antioxidants on the skin immune system. Earlier studies from our laboratory have demonstrated that short-term (i.e., 5-day daily) topical applications
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)