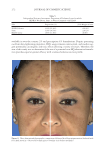
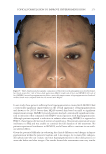
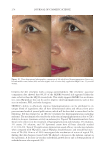
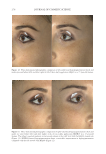
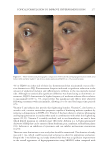
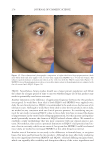
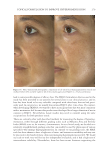
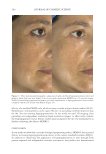
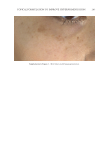
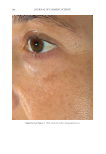
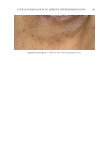
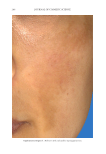
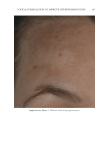
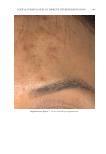
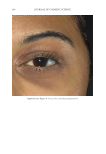
JOURNAL OF COSMETIC SCIENCE 280 effi cacy of a modifi ed MASI scale, which we may consider using in future studies (40,41). Furthermore, chromameters can be quite effective in providing excellent objective data for the clinician treating hyperpigmentation. In our study, we used 3D imaging, thus providing our independent evaluators high-resolution images to effectively evaluate the hyperpigmented areas. Future studies may incorporate the use of a chromometer in further evaluating the effi cacy SKNB19. C ONCLUSION I n our study, we show that a recently developed proprietary product, SKNB19, has increased effi cacy in treating hyperpigmentation relative to the current standard treatment HQ4%. In addition to improving the appearance of hyperpigmentation as seen through both patient-reported and independent reviewer assessments, the product also demonstrated Figure 17. Three-dimensional photographic comparison of right-sided facial hyperpigmentation (cheek and midface) before (left) and after (right) 4 wk of twice-daily application SKNB19 in a 53-year-old woman. SKNB19-treated hyperpigmentation shows a noticeable improvement in hyperpigmentation more so when compared with the side treated with HQ4% (Figure 16).
TOPICAL FORMULATION TO IMPROVE HYPERPIGMENTATION 281 better tolerability, as well as reduced redness and irritation relative to HQ4%. This prod- uct has been found to be safe and effective for use in hyperpigmentation. R EFERENCES (1) N. A. Vashi and R. V. Kundu, Facial hyperpigmentation: causes and treatment, Br. J. Dermatol., 169(Suppl 3), 41–56 (2013). (2 ) D. Rigopoulos, S. Gregoriou, and A. Katsambas, Hyperpigmentation and melasma, J. Cosmet. Dermatol., 6, 195–202 (2007). (3 ) A. K. Gupta, M. D. Gover, K. Nouri, and S. Taylor, The treatment of melasma: a review of clinical tri- als, J. Am. Acad. Dermatol., 55, 1048–1065 (2006). (4 ) S. Yanagishita-Nakatsuji, K. Fukai, A. Ohyama, A. Umekoji, J. Sowa-Osako, and D. Tsuruta, Probable allergic contact dermatitis from hydroquinone presenting as leukomelanoderma: report of two cases, J. Dermatol., 44, e330–e331 (2017). (5) S. N. Mishra, R. S. Dhurat, D. J. Deshpande, and C. S. Nayak, Diagnostic utility of dermatoscopy in hydroquinone- induced exogenous ochronosis, Int. J. Dermatol., 52, 413–417 (2013). (6 ) F. W. Kari, J. Bucher, S. L. Eustis, J. K. Haseman, and J. E. Huff, Toxicity and carcinogenicity of hy- droquinone in F344/N ratsand B6C3F1 mice, Food Chem. Toxicol., 30, 737–747 (1992). (7 ) T. Tsutsui, N. Hayashi, H. Maizumi, J. Huff, and J. C. Barrett, Benzene-, catechol-, hydroquinone- and phenol-induced cell transformation, gene mutations, chromosome aberrations, aneuploidy, sister chroma- tid exchanges and unscheduled DNA synthesis in Syrian hamster embryo cells, Mutat. Res., 373, 113–123 (1997). (8 ) M. H. Yu and S. O. Lee, Hydroquinone stimulates cell invasion through activator protein-1-dependent induction of MMP-9 in HepG2 human hepatoma cells, Food Chem. Toxicol., 89, 120–125 (2016). (9) V. M. Sheth and A. G. Pandya, Melasma: a comprehensive update: part II, J. Am. Acad. Dermatol., 65, 699–714 (2011). (1 0) N. Atefi , B. Dalvand, M. Ghassemi, G. Mehran, and A. Heydarian, Therapeutic effects of topical tranexamic acid in comparison with hydroquinone in treatment of women with melasma. Dermatol. Ther (Heidelb)., 7, 417–424 (2017). (1 1) M. Banihashemi, N. Zabolinejad, M. R. Jaafari, M. Salehi, and A. Jabari, Comparison of therapeutic effects of liposomal tranexamic acid and conventional hydroquinone on melasma, J. Cosmet. Dermatol., 14, 174–177 (2015). (1 2) M. S. Janney, R. Subramaniyan, R. Dabas, S. Lal, N. M. Das, and S. K. Godara, A randomized controlled study comparing the effi cacy of topical 5% tranexamic acid solution versus 3% hydroquinone cream in melasma, J. Cutan. Aesthetic Surg., 12, 63–67 (2019). (1 3 ) B. Ebrahimi and F. F. Naeini, Topical tranexamic acid as a promising treatment for melasma, J. Res. Med. Sci., 19, 753–757 (2014). (1 4 ) M. Martínez-Esparza, C. Ferrer, M. T. Castells, J. C. García-Borrón, and A. Zuastiand, Transforming growth factor beta1 mediates hypopigmentation of B16 mouse melanoma cells by inhibition of melanin formation and melanosome maturation, Int. J. Biochem. Cell Biol., 33, 971–983 (2001). (15) M. Brenner and V. J. Heari n g, Modifying skin pigmentation - approaches through intrinsic biochemis- try and exogenous agents, Drug Discov. Today Dis. Mech., 5, e189–e199 (2008). (16) H. Kim, H. R. Choi, D. S. K im, and K. C. Park, Topical hypopigmenting agents for pigmentary disor- ders and their mechanisms of action, Ann. Dermatol., 24, 1–6 (2012). (17) G. H. Park, Y. Rhee do, H. R. Moon, C. H. Won, M. W. Lee, J. H. Choi, K. C. Moon, and S. E. Chang, Effect of an epidermal growth factor-containing cream on postinfl ammatory hyperpigmentation after Q-switched 532-nm neodymium-doped yttrium aluminum garnet laser treatment, Dermatol. Surg., 41, 131–135 (2015). (18) D. Steiner, C. Feola, N. B i aleski, F. A. Silva, A. C. P. Antiori, F. Addor, and B. B. Folino, Study evaluat- ing the effi cacy of topical and injected tranexamic acid in treatment of melasma, Surg. Cosmet. Dermatol., 1, 174–177 (2009). (19) P. Kanechorn Na Ayuthaya, N . Niumphradit, A. Manosroi, and A. Nakakes, Topical 5% tranexamic acid for the treatment of melasma in Asians: a double-blind randomized controlled clinical trial, J. Cosmet. Laser Ther., 14, 150–154 (2012). (20) S. J. Kim, J. Y. Park, T. S hibata, R. Fujiwara, and H. Y. Kang, Effi cacy and possible mechanisms of topical tranexamic acid in melasma. Clin. Exp. Dermatol., 41, 480–485 (2016).
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)