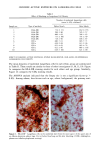
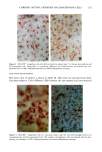
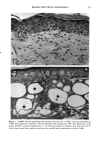
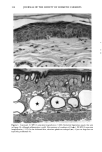
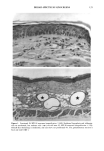
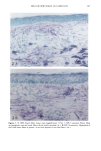
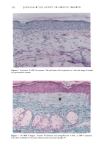
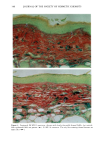
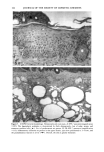
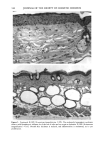
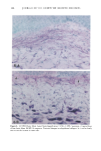
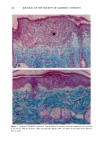
152 JOURNAL OF THE SOCIETY OF COSMETIC CHEMISTS Table III Skin Thickness (•) - SEM (n = 6) Sunscreen group 10 MPD 16 MPD SPF-7 626.7 + 30.1 a 783.8 + 41.7 a SPF-16 586.3 + 16.4 a 782.0 + 32.7 a SPF-18 516.8 + 9.5 b 546.3 --- 29.1 c Compared to unirradiated controls (461 -+ 9.1 •): ap = 0.002 bp ---- 0.004 Cp = 0.04. Mann-Whitney two-sample test (two-tailed). Table IV Tumors Present After 16 MPD* Group Mouse No. Description SPF-7 3731 1: 1-mm papilloma 3735 1: 2-mm papilloma 1: 5-mm tumor 2: cystic lesions 3736 1: 2-mm papilloma 3764 SPF- 16 1: 2-mm papilloma (low on flank) * After 10 MPD, no tumors were present on any of the mice. absorber Parsol 1789 (330-400 nm peak absorption 355 nm), provided the most effective protection. Epidermal and dermal damage occurred albeit to a lesser extent than with the other sunscreens. As might be expected, photodamage in all groups was greater at the 16 MPD end point than at t0 MPDs. Notably, there was less progressive damage with time and increased MPDs in the SPF-18 group than in the other two groups. It should be made clear that the level of damage incurred with 7 MEDs of chronic exposure of sunscreen-protected mice was considerably less than that seen in unprotected mice from our data base. These controls were exposed to --1.5 MED of SSR thrice weekly for --30 weeks (10). Under these conditions elastosis was more severe, loss of collagen staining was extensive, and GAGs were greatly increased with a deposition pattern characteristic of both UVB and UVA exposure. Dermal cysts had proliferated up to six rows. In a previous photocarcinogenesis study with unprotected mice exposed to t MED of SSR for only ten weeks, tumor incidence was 100% at week 27, with --7 tumors/mouse (15). This contrasts strongly with the tumor data from the present study in which no tumors developed in the SPF-18 sunscreen group. Even in the SPF-7 sunscreen group, only three of the nine surviving mice developed one or two small tumors. Evidence of chronic suberythemal UVB damage was seen especially with the SPF-7 sunscreen as loss of affinity for the collagen-specific stain. We have shown previously (t0) that even large doses of UVA do not produce this histologic change. The appearance of stippled-blue-staining GAGs at both dose points in the SPF-7 and SPF-16 protected groups also suggests UVB effects (3, t0). UVA damage was characterized in all groups at 16 MPDs by the focal bluish tone imparted to the collagen as if the bundles were coated with GAGs. This tinctorial change does not occur with UVB (10). Also indic-
BROAD-SPECTRUM SUNSCREENS 153 ative of UVA-induced damage were the dense GAG deposits at the dermal-epidermal junction, especially prominent at 16 MPD (10). With stains for general morphology (H&E) and elastic fibers, it was not possible to distinguish between UVB and UVA effects. It is likely that transmitted radiation from both broad wave bands contributed to the observed damage. Effects of suberythemal UV doses have also been reported in human studies. Our observation of sunburn cells (SBCs) in most specimens at both dose points, regardless of the SPF of the sunscreen, confirms findings by Kaidbey in acute studies (16). Human subjects, pretreated with an SPF-15 sunscreen, were exposed to an SSR dose equal to the previously determined SPF of the product on each individual. Subjects were also treated with an SPF-30 sunscreen and irradiated with 15 MEDs. Faint erythema developed in some of the SPF-15 protected sites but not in the SPF-30 sites. Although the greatest number of SBCs occurred in the SPF-15 protected group, SBCs were induced in all subjects and with both sunscreens. Thus, injury to epidermal cells can occur in the absence of erythema and with UV doses that are far below the SPF of the sunscreen. In a different approach, but nevertheless demonstrating the effects of suberythemal radiation, Lavker et al. (17) exposed human subjects, at different sites, to 0.5 MED of SSR (290-400 nm) and 0.5 MED of UVA (320-400 nm) over a period of 5 ¾2 weeks for 28 doses. Notable changes compared to unirradiated skin were increased binding of lysozyme to elastic fibers, which suggests some change in the fibers, and increased inflammatory cells as visualized by leukocyte common antigen deposition. Similar changes were produced by both spectra, with the greatest effect seen with UVA. These studies, including our present findings, attest to the fact that structural components of skin can be damaged with far less radiation than it takes to produce a sunburn. In contrast to the evidence from our study, it has been proposed, from theoretical considerations, that the amount of UVA radiation transmitted through high-SPF sun- screens is not a significant factor in chronic photodamage (18). This a, gument derives from calculations based on acute exposure with erythema as the end point without considering the diverse biologic consequences of chronic exposure over decades. •', also fails to take into account the low absorbance capacity of some UVA II absorbers and the long-term effects of UVA on dermal matrix damage. For a UVA protection factor to be such that it is capable mainly of preventing an MED of UVA-induced erythema during the exposure period is not supported by in vivo experiments that show skin damage at suberythemal UVA doses. The claim that skin damage from 150 minutes of protected exposure with an SPF-15 sunscreen would be the same as from ten minutes of unpro- tected exposure (18) is therefore true only with respect to erythema. Recent research has demonstrated that although UVB is the most damaging portion of the sunlight reaching earth, UVA is responsible for numerous molecular and biochem- ical events that contribute to photodamage in skin (19-21). There is little dispute that both UVB and UVA contribute to chronic photodamage. Additionally, the effects of long-term UVA radiation are qualitatively and quantitatively quite different from those of UVB (10,22,23). Thus, protection against both broad wave bands is needed. The concept that prevention of sunburn is sufficient needs to be reexamined in light of the multiple effects demonstrated in this study of both UVB and UVA in the absence of erythema. Moreover, as our data show, extending protection well into the UVA I region with the addition of avobenzone to the octyl methoxycinnamate-oxybenzone sunscreen
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)