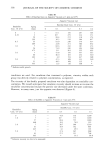
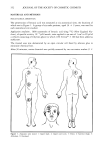
324 JOURNAL OF THE SOCIETY OF COSMETIC CHEMISTS I o o o 12 8 soAP A k• •'... "-..... . .•- SOAP D 4 u.•roo•oa x • " ' ............ 27777 2 x ....... ! ! ! ! i ! ! ! Figure 6. Fluorescence of skin surface after treatment with soaps (0.75%) followed by Rhodamine B. c 1.5 SOAP D Woto• SOAP A EXTRACTING MEDIUM Figure 7. Quantities of ninhydrin-positive material extracted from skin by soap solutions.
CLEANSING BAR EVALUATION 325 is eliminated within a few hours (Figure 1) and limited to the upper horny layer (Figure 5). This means that the buffer capacity of the horny layer by far exceeds the amount of acid necessary to transform residues of surfactant-like soaps to fatty acids. These fatty acids are natural ingredients of skin surface (16, 17) and epidermal lipids (18). In contrast to this, the application of 100 p•l of 8% solution of soaps to a 1-cm 2 skin site under occlusive conditions causes a pH shift which lasts for more than 24 hours. There- fore, the applied quantity by far exceeds the buffer capacity of the treated horny layer. Under these circumstances the irritating molecular species are totally different from those which can possibly penetrate into skin during normal product use. Surfactants do not undergo such changes and their surface activity is rather independent of the pH value of the surrounding medium. Therefore, it must be concluded that a comparison of irritancy of soaps and surfactants via patch tests neglects the deactivation of soaps to fatty acids (likely to take place during normal product use) by overwhelming the buffer capacity of the skin's acid mantle. Normal unoccluded skin shows a pH shift from 5.5 to 6.8 after removal of 15 layers by stripping (19). Occlusion of skin for five days causes a steady increase of surface pH values from weakly acid to neutral values (20), probably due to equilibration of the horny layer with the interstitial fluid. Therefore, occlusion under Finn chambers will potentlate the adverse effects of a classical soap by shifting upward the skin surface pH. After application of the soaps, the skin surface remains depleted of pH-buffering sub- stances. There is no significant effect on the extracted tissue due to differences in pH values of 5-6 compared to 7-8. In both cases the buffer capacity of the skin surface is lowered and has to be restored during the following hours. This point of view is confirmed by the results of the investigation concerning the skin- care effect due to regular use of the soaps. The roughness of skin sites routinely treated with D is comparable to that treated with A and significantly smoother than that treated with B or C. Fissures which increase roughness values are one of the criteria which contribute to the scores describing the degree of skin damage after patch testing. Under the conditions of regular use, D and A apparently improve or do not worsen (Table VII) skin surface structure (21). The rate of water loss, which is another aspect of the structural integrity of the horny layer, was lower after treatment with classical soaps compared to treatment with A. An explanation may be found in Table VIII. Whereas skin treated with classical soaps deactivates soap anions (which certainly can enhance skin permeability (7) very quickly, surfactants remain unchanged and have to be eliminated by desquamation, permeation into deeper skin layers, microbial degradation, or mechanical wear-off. Generally, an- ionic surfactants including soaps are more irritating than water-insoluble lipids. Permeation of A is detectable up to at least eleven strips deep, while the traces of D disappear gradually after removal of six strips (Figure 6). The lowering of charge density of "untreated" sites after washing with water may be caused by removal of surfactants which might be the residues of preceding daily cleansing activities. The molecular identities of the fluorophors responsible for the phenomena described in Figure 4 are still unknown. Nevertheless, it is plausible that NADH contributes mainly to the signal excited at 360 nm and that it will be reduced in relation to the degree of inflammation (Table IV) (22 a/b).
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)