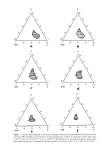
PREPRINTS OF THE 1998 ANNUAL SCIENTIFIC MEETING 71 HUMAN NAIL AND ITS TOPICAL TREATMENT: BRIEF REVIEW OF CURRENT RESEARCH AND DEVELOPMENT OF TOPICAL ANTIFUNGAL DRUG DELIVERY FOR ONYCHOMYCOSIS TREATMENT Jonas C.T. Wang and Ting Sun, Ph.D. Johnson and Johnson Topical Formulation and Drug Delivery Technology Resource Center, Johnson and Johnson Consumer Products, Skillman, New Jersey, USA Biochemical Properties of the Nail The human nail plate is composed of approximately 25 layers of flattened, keratinized cells fused into a dense, hard yet slightly elastic plate, with a typical thickness of 0.5 - 1.0 mm (1). These cells have their origin in the nail matrix, a living highly proliferative epithelia tissue (Figure 1). Human nail compared with human stratum corneum has less lipid (1% versus 20%) and higher percentage of disulfide linkages (10.6% versus 1.2%) also is thicker (750 p versus 30p) but holds less water (25% versus 300%) (ref. 2-4). The high disulfide bond content confers toughness to the nail (3). Nail consists of three layers (Figure 1): (i) hard dorsal nail plate 0.Smm thick in finger nails and 1.3mm for toe nails, (ii) nail bed of noncornified soft tissue, and (iii) nail matrix which is the thick, highly proliferative tissue at the root of the nail. History of Topical Nail Delivery In contrast to the abundant literature available on chemical skin penetration enhancers, information on chemical nail penetration enhancers is rather scarce. Due to the different nature of the barriers, the likelihood of success would not be very high if one simply used a proven-effective skin penetration enhancer for nail delivery. The working mechanism for a vast majority of skin penetration enhancers involves the lipid domains or pathways in the stratum corneum., either by increasing the fluidity, or by increasing the drag partitioning into it. These skin penetration enhancers are unlikely to have the same penetration enhancement effect on the nail simply because the nail contains much less lipid, probably has much less well-developed lipid pathways. The aforementioned differences between the nail and stratum corneum, both physical and chemical, are probably responsible for the lack of efficacy of the topical nail antifungal products on the market (5), as well as for the ineffectiveness of some well known skin penetration enhancers, such as dimethyl sulfoxide and homologous alcohols, on nail permeation enhancement (6). Walters and his associates (2, 6, 7) discovered that, as a permeation barrier, a human nailplate does not mimic the behavior of a lipophilic membrane, which has been the case for almost all the other body membranes, such as the skin, vaginal and gastrointestinal mucousal membranes. Instead a hydrated nail plate behaves more like a hydrogel membrane in its barrier properties. Mertin and Lippold (7,8,9) pointed oat that for onychomycosis treatment (nail fungal infections), not only the flux of an antimycotic drag through the nail plate is of
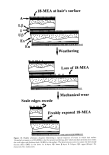
72 JOURNAL OF COSMETIC SCIENCE importance, but also the antifungal potency, which expressed as minimum inhibitory concentration (MIC). An efficacy coefficient E is therefore introduced, which should be maximum for high ther.apeutie effectiveness (9): E = Flux \ MIC Thus one wishes to obtain a high flux of drug through the nail and a low MIC for maximum efficacy. Flux is also directly proportional to molecular size of the drug(9). Recent Progress of the Research of Topical Drug Delivery to the Nail for Onyehomyeosis Treatment Fungal infections of the nails (onychomycosis) makes up about 30% of fungus infections of the skin. Onychomycosis involves about 2-5% of general population. Of the 245 million people in the United States, between 4.9 and 12.3 million are infected with onychomycosis. Onychomycosis takes a profound psychosocial toll on the sufferer. Although there are many potent antifungal drugs currently available, nail fungal infections remain a disease very difficult to treat. In the U.S., only oral administration of three antifungal drugs is approved by FDA as effective therapy for nail fungal infection: itraconazole (Sporanox©), terbinafine (Lamisil©), and an old drug, griseofulvin. Because of the long duration of oral treatment for onychomycosis (3-12 months), potential adverse effects, such as hepatotoxicity and drug interactions, are often of concern. In addition, relapse rate is rather high. To minimize the undesirable side effects associated with systemic treatment, it is highly desirable to have an efficacious topical product to treat onychomycosis. However, ability for a topical drug to penetrate the nail plate has hampered this approach. Keratolyic agents, such as urea and salicylic acid are often used to soften nail plates. Urea and a combination of urea and salicylic acid were reported to be used for nonsurgical avulsion of nail dystrophies in clinical studies prior to topical treatment of onyehomyeosis with satisfactory results (10-12). Lauharanta (13) reported another favorable clinical study of using an amorolfine-containing nail lacquer (Loeeryl nail lacquer} with a special nail preparation procedure (cleaning, filing and cutting} to treat onyehomyeosis in clinical trials. Clinical trials demonstrated that this special procedure was essential. The physical elimination of a part of the nail barrier certainly facilitated the drug penetration for a better efficacy. Similar results were also observed from a Cilcopirox lacauer product. By exploiting target sites on the nail keratin (Figure 2), we discovered a novel way of using chemical enhancers that act directly on the nail keratin to increase nail elasticity, and consequently, to enhance drug permeation through the nail (14). Certain sulfhydryl compounds, such as cysteine, a natural amino acid, or its derivative acetylcysteine (NAC), cleave the disulfide bonds of nail keratin. Urea was used to interact with hydrogen bonds of nail keratin to facilitate the disulfide bond breaking (Figure 2). The chemical reaction that occurs between the cystinc linkages in nail keratin and cysteine is
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)