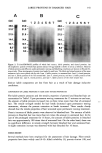
PHOSPHATIDYLCHOLINE AS PENETRATION ENHANCER 373 3OO 250 •- 200 o "• 150 E Q- 100 o• 50 = 1% PC ......... • .... 2% PC + 4%PC 0 5 10 15 20 25 Time(hr) Figure 9. Effect of phosphatidylcholine concentration on the skin permeation of caffeine. can be interpreted that phosphatidylcholine itself can act as a permeation enhancer, its mechanism more closely connected with modulating skin barrier function than with vesicular delivery. In fact, most of the caffeine molecules in the formulation were located in the continuous phase and not in the vesicles because of caffeine's water solubility and leakage from the vesicles. Oil-soluble materials may lead to different results because they tend to remain in the vesicles. However, phosphatidylcholine is a reliable, mild, skin permeation enhancer that can be used in cosmetic products. REFERENCES (1) J. L. Zatz, Optimizing skin delivery, Cosmet. Toiletr. 115, 31-35 (2000). (2) J. W. Wiechers, Avoiding transdermal cosmetic delivery, Cosmet. Toilerr. 115, 39-46 (2000). (3) S. Magdassi and E. Touitou, Novel Cosmetic Delivery Systems (Marcel Dekker, New York, 1999), pp. 1-97. (4) Y. Yokomizo and H. Sagitani, Effects of phospholipids on the percutaneous penetration of indometh- acin through the dorsal skin of guinea pigs in vitro, J. Contr. ReL, 38, 267-274 (1996). (5) Y. Yokomizo and H. Sagitani, The effects of phospholipids on the percutaneous penetration of indomethacin through the dorsal skin of guinea pig in vitro. 2. The effects of the hydrophobic group in phospholipids and a comparison with general enhancers, J. Contr. ReL, 42, 37-46 (1996).
374 JOURNAL OF COSMETIC SCIENCE (6) (7) (8) (9) (10) (11) (12) (13) (14) (15) (16) (17) H. Schreier, and J. Bouwstra, Liposomes and niosomes as topical drug carriers: Dermal and transdermal drug delivery, J. Contr. Rel., 30, 1-15 (1994). G. Cevc and G. Blume, Lipid vesicles penetrate into intact skin owing to the transdermal osmotic gradient and hydration force, Biochim. Biophys. Acta, 1104, 226-232 (1992). G. M. E1 Maghraby, A. C. Williams, and B. W. Barry, Skin delivery of oestradiol from deformable and traditional liposomes: Mechanistic studies, J. Pharm. Pharmacol., 51, 1123-1134 (1999). G. M. E1 Maghraby, A. C. Williams, and B. W. Barry, Skin delivery of oestradiol from lipid vesicles: Importance of liposome structure, Int. J. Pharm., 204, 159-169 (2000). H. Sasaki, M. Kojima, J. Nakamura, and J. Shibasaki, Acute toxicity and skin irritation of pyrrolidone derivatives as transdermal penetration enhancer, Chem. Pharm. Bull., 38, 2308-2310 (1990). T. K. Ghosh, W. R. Pfister, and S. I. Yum, Transdermal and Topical Drug Delivery System (Interpharm Press, Buffalo Grove, Ill., 1997), pp. 191-214. E. Mayhew, R. Lazo, W. J. Vail, J. King, and A.M. Green, Characterization of liposomes prepared using a microemulsifier, Biochim. Biophys. Acta, 775, 169-174 (1984). J. C. Vuillemard, Recent advances in the large-scale production of lipid vesicles for use in food products: Microfluidization, J. Microencapsul., 8, 547-562 (1991). D. W. Fry, J. C. White and I. D. Goldman, Rapid separation of low molecular weight solutes from liposomes without dilution, J. Anal. Biochem., 90, 809-815 (1978). M. Kirjavainen, A. Urtti, R. Valjakka-Koskela, J. Kiesvaara, and J. M6nkk6nen, Liposome-skin interactions and their effects on the skin permeation of drugs, Eur. J. Pharm. Sci., 58, 207-217 (1999). F. P. Bonnia, L. Montenegro, N. Scrofani, et al., Effects of phospholipid based formulations on in vitro and in vivo percutaneous absorption of methyl nicotinate, J. Contr. Rel., 34, 53-63 (1995). M. Kirjavainen, J. M6nkk6nen, M. Saukkosaari, R. Valjakka-Koskela, J. Kiesvaara, and A. Urtti, Phospholipids affect stratum corneum lipid bilayer fluidity and drug portioning into the bilayers, J. Contr. Rel., 58, 207-214 (1999).
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)