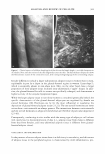
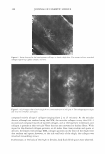
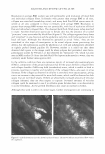
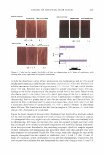
430 JOURNAL OF COSMETIC SCIENCE Then three test sites were designated on the lateral aspect of one lower leg of each subject, and two test sites on the other. Each site measured 5 cm by 5 cm. To be included in the study, panelists had to show a dryness score of 2::2.5 on a 0-to-4 scale (see below) on all the test sites. A trained evaluator performed all dry skin evalu ations in a blinded manner. Baseline (Day 0) measurements were then taken (Table II). Measurements using a Skicon® 200 conductance meter with an MT probe were taken in triplicate at each site on each participant by a trained operator. D-Squames® tape was then used to sample the dry flaky skin. Each test area was sub-divided into four quadrants. Each quadrant was sampled once with a D-Squames® disc during the study. Three samples were taken for determination of the desquamation index (DI) and a fourth sample for squamometry on Day 4. To sample the skin, a D-Squames® (25-mm) disc was applied to the designated site and a plunger was used to apply a constant pressure. Each D-Squames® disc was then removed and affixed to a black, labeled card. The D-Squames® discs were evaluated by computerized image analysis according to the method of Schatz et al. (11) to yield the desquamation index (DI). Test lotions were assigned to the sites using a balanced complete-block design, i.e., each panelist was treated with all the test products and had a "no product" control site. The assignment of the test products to individual test sites was balanced between panelists. To each site, a technician, using a finger cot, applied 0.05 ml of the assigned test lotion (dosage = 2 mg/cm2). A total of eight test lotion applications were made, twice daily, at least three hours apart, on Days 0, 1, 2, and 3. Treatment was followed by a regression period of four days, during which moisturizing products could not be used on the legs. Thus, the duration of the study totaled eight days. For both the treatment period and the regression period, subjects were directed to wash their legs only with Ivory® soap. Panelists were to wash their lower legs each morning using their normal procedure similarly on each leg otherwise the participants were to refrain from wetting their legs. On evaluation days (Days 0, 4, and 7), panelists were instructed that washing was to be at least two hours before the first visit of the day. Each test site was re-evaluated for observer scoring, desquamation index, and conduc tance on Days 4 and 7. Additionally, on Day 4, a second set of D-Squames® was taken and used for squamometry readings. Statistics. Skin hydration (conductance) and the desquamation index (DI), provided the primary measures of product efficacy. Visual evaluations and color readings of the stained D-Squames® provided secondary measures of efficacy. For skin hydration, observable Dryness score* 0 1 2 3 4 * Half scores permitted. Table II Dryness Scoring Scale Description of skin No dryness Slight flaking Moderate flaking/scaling Marked scaling/slight fissuring Severe scaling/fissuring A photographic scale was provided to illustrate examples of each dryness score.
MOISTURIZER EFFICACY 431 dryness, and D.I., the effects of the test products were compared with each other and the "no product" control, using "change from baseline" data. Comparison with the "no product" control represented the effect of the product on the skin. By comparing the subsequent "no product" control readings to the baseline (Day 0), we can assess the effects of the environment on the skin. For, skin hydration, DI, and observer (visual) scoring of scaling, a two-way (time x product) repeated-measure ANOVA was run using the "change from baseline" data. When an overall significant difference (p ::::::: 0.05) was detected, the products and the untreated site were compared using the Tukey HSD test. For stained D-Squames®, statistical analyses reflected the differences between treated sites and the "no product" control site using a one-way, within-subject, ANOV A. If an overall significant difference was detected (p ::::::: 0.05), then the significance of the differences between the lotions, as well as between the untreated sites, was assessed using the Tukey HSD test. MODEL SYSTEM II. BENEFIT: PREVENTION OF DRYNESS HAND-WASH TEST Test history. Repeated exposure to surfactants and water is a major cause of dry skin and eczema. Professions such as health care, hairdressing, and food preparation have elevated rates of eczema (12). Indeed, Nilsson et al. (13) found that nurses who wash their hands frequently have double the rate of hand eczema of a balanced cohort of clerical workers. Atopy also increased the probability of the occurrence of eczema. The hand wash meth odology developed by Highley et al. (1) was selected as the model to assess the ability of moisturizers to prevent the induction of dryness. It is also possible to induce erythema and stratum cornuem damage, but this requires more handwashes than required to produce dryness (14). For this study, the design of Highley et al. was significantly updated. Instead of small study groups (n = 5), larger groups of panelists (n 2:: 25) were employed to allow for the use of better statistical methods. Furthermore, the effectiveness of multiple moisturizers was compared by trained observers, augmented with biophysical methods such as skin conductance and squamometry not available at the time of Highley' s publication. Current procedure. Thirty male and female subjects between the ages of 18 and 65 par ticipated in this study. Panelists were in good health other than having a tendency to develop dry skin on their hands. Participants were provided with Dial® liquid soap at the beginning of the study and throughout the study. Except for using Dial® liquid soap, participants were not allowed to use any other soaps, moisturizers, creams, or lotions on the backs of their hands until the study was completed. For activities in which the backs of the hands might contact another soap or detergent, panelists were to wear the rubber gloves provided. These restrictions were imposed three days before the start of the treatment phase of the study. At the beginning of the treatment phase, the baseline condition of the skin was deter mined. Panelists sat at rest in an environmentally controlled room (temperature :::::::21 °C, RH = 3 5 ± 10%) for at least 15 minutes. Once acclimated, a trained observer evaluated the skin on the back of each subject's hands using a 0-4 categorical scale for skin scaling.
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)