262 JOURNAL OF COSMETIC SCIENCE CONCLUSIONS A controlled application protocol for testing a unique moisturizer form, the in-shower body lotion, was developed based on an understanding of consumer habits and practices related to showering and in-shower body lotion use. This work demonstrates that this in-shower body lotion test protocol is valid, i.e., it reliably discriminates among prod ucts that are known to deliver different levels of moisturization and yields reproducible results upon product retest. Further, the results from studies conducted during protocol development show that the petrolatum-depositing in-shower body lotion products tested are robust in terms of their ability to provide a dry skin benefit across a range of consumer-relevant use conditions. REFERENCES (1) C. L. Froebe, F. A. Simion, H. Ohlmeyer, L. D. Rhein, J. Mattai, R.H. Cagan, and S. E. Friberg, Prevention of stratum corneum lipid phase transitions in vitro by glycerol-An alternative mechanism for skin moisturization, J. Soc. Cosmet. Chem., 41, 51-65 (1990). (2) A. Rawlings, C. Harding, A. Watkinson, J. Banks, C. Ackerman, and R. Sabin, The effect of glycerol and humidity on desmosome degradation in stratum corneum, Arch. Dermatol. Res., 287(5), 457-464 (1995). (3) 0. Tanno, Y. Ota, N. Kitamura, T. Katsube, and S. Inoue, Nicotinamide increases biosynthesis of ceramides as well as other stratum corneum lipids to improve the epidermal permeability barrier, Br. J. Dermatol., 143(3), 524-531 (2000). (4) M. Mao-Qiang, B. E. Brown, S. Wu-Pong, K. R. Feingold, and P. M. Elias, Exogenous nonphysiologic vs physiologic lipids: Divergent mechanisms for correction of permeability barrier dysfunction, Arch. Dermatol., 131(7), 809-816 (1995). (5) J. Bikowski, The use of therapeutic moisturizers in various dermatologic disorders, Cutis, 68(Suppl. 5), 3-11 (2001). (6) A. W. Lucky, A. D. Leach, P. Laskarzewski, and H. Wenck, Use of an emollient as a steroid-sparing agent in the treatment of mild to moderate atopic dermatitis in children, Pediatr. Dermatol., 14(4), 321-324 (1997). (7) Y. Soma, M. Kashima, A. Imaizumi, H. Takahama, T. Kawakami, and M. Mizoguchi, Moisturizing effects of topical nicotinamide on atopic dry skin, Int. J. Dermatol., 44(3), 197-202 (2005). (8) American Academy of Dermatology. Winterize Your Skin: Dermatologists' Top Tips for Surviving the Cold [Internet} October 22, 2003 [cited August 4, 2007}. Available from: http://www.aad.org/public/ N ews/N ewsReleases/Press +Release+Archives/General+Skin+Care/WinterSkinBaumann.htm. (9) J. Hanifin and S. C. Chan, Diagnosis and treatment of atopic dermatitis, Dermatol. Ther., l, 9-18 (1996). (10) K. L. Hon, T. F. Leung, Y. Wong, H.K. So, A. M. Li, and T. F. Fok, A survey of bathing and showering practices in children with atopic eczema, Clin. Exp. Dermatol., 30(4), 351-354 (2005). (11) W. E. Roberts, K. D. Ettel, P. M. Hartwig, R. A. Bacon, V. Rodriguez, and R. D. Farris, Breaking the cycle of dry body skin through effective product design, 62nd Annual Meetinf!, of the American Academy of Dermatology, Washington, DC, February 6-111 2004. (12) K. D. Ertel, P. B. Neumann, P. M. Hartwig, G. Y. Rains, and B. H. Keswick, Leg wash protocol to assess the skin moisturization potential of personal cleansers, Int.]. Cosmet. Sci., 21, 383-397 (1999). (13) United States Environmental Protection Agency, Exposure Factors Handbook, National Center for En vironmental Assessment Office of Research and Development, United States Environmental Protection Agency, Rockville, MD, Chapter 6-Dermal, 2007. Available from: http://www.epa.gov/oppt/ exposure/presentations/efast/use_l 997 _efb.pdf. (14) R. M. Azurdia, J. A. Pagliaro, B. L. Diffey, and L. E. Rhodes, Sunscreen application by photosensitive patients is inadequate for protection, Br. J. Dermatol., 140(2), 255-2'58 (1999). (15) N. Bech-Thonsen and H. C. Wulf, Sunbathers' application of sunscreen is probably inadequate to obain the sun protection factor assigned to the preparation, Photodermatol. Photoimmunol. Photomed., 9, 242-244 (1993).
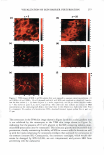
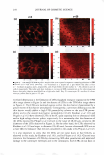
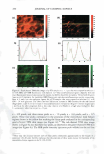
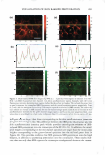
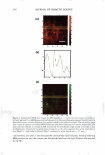
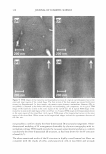
J. Cosmet. Sci., 59, 263-289 Ouly/August 2008) Visualization and quantification of skin barrier perturbation induced by surfactant-humectant systems using two-photon fluorescence microscopy SASWATA GHOSH, DAEKEUN KIM, PETER SO, and DANIEL BLANKSCHTEIN, Departments of Chemical Engineering (S.G., D.B.) and Mechanical Engineering (D.K., P.S.), Massachusetts Institute of Technology, Cambridge, MA 0213 9. Accepted for publication February 20, 2008. Synopsis In order to visualize the effects of aqueous surfactant-humectant systems on the skin barrier, an in vitro two-photon fluorescence microscopy (TPM) study, including dual-channel visualization, was carried out. TPM is a non-invasive imaging technique based on two-photon induced nonlinear excitations of fluoro phores, with the capability for deep-tissue imaging (up to several hundred micrometers). The following aqueous solutions of surfactants, a humectant, and a surfactant+humectant mixture that contacted pig full-thickness skin (p-FTS) were studied: (i) a harsh surfactant solution-sodium dodecyl sulfate (SDS) (1 wt%) (ii) a harsh surfactant+humectant solution-SDS (1 wt%) + glycerol (10 wt%) (iii) a mild surfactant solution-sodium cocoyl isethionate (SCI) (1 wt%) (iv) a control solution-phosphate-buffered saline (PBS) and (v) a humectant solution-glycerol (10 wt%). Sulforhodamine B (SRB), a hydrophilic fluorescent probe, was used to visualize the effects of aqueous contacting solutions i - on the skin barrier morphology. The results of the TPM visualization study revealed that SDS induces corneocyte damage by denaturing keratins and creating intracorneocyte penetration pathways. On the other hand, SDS+glycerol did not significantly induce corneocyte damage. The dual-channel TPM images corresponding to aqueous contact ing solutions iii-v showed low SRB penetration into the corneocytes, as well as localization of the SRB probe within the lipid bilayers surrounding the corneocytes of the SC. Through a quantification of the amount of SRB that penetrated into the skin as a function of skin depth, we found that adding glycerol to an SDS aqueous contacting solution can significantly reduce the SDS-induced penetration depth of SRB, which provides evidence of the ability of glycerol to mitigate SDS-induced skin barrier perturbation. The distri bution of SRB in the p-FTS samples was analyzed using a theoretical model that quantified changes in the skin aqueous pore characteristics induced by aqueous contacting solutions i, ii, iii, and v, relative to aqueous contacting solution iv, the control. The results of the theoretical model indicate the following ranking order in the extent of perturbation to the skin aqueous pores (from the highest to the lowest): i ii iii iv v. The development of such an in vitro visual ranking methodology, including quantification using TPM, can potentially reduce mariy costly in vivo screening procedures, thereby significantly reducing the cost and time-to-market of new cosmetic formulations containing surfactants and humectants. INTRODUCTION Surfactants are commonly used in skin cleansing formulations because of their ability to stabilize oil-water emulsions and clean the surface of the skin. However, some surfac- Address all correspondence to Daniel Blankschtein. 263
Purchased for the exclusive use of nofirst nolast (unknown) From: SCC Media Library & Resource Center (library.scconline.org)